Managing Up Your Clinical Team Improving Communication Between Hospital Medicine and Specialist Teams

As we ring in the new year, we take a moment to reflect on the past and recommit to the things that matter the most. In that light, this issue of Rx for PX focuses on the tenets and importance of patient satisfaction: empathy, efficiency, a service attitude, and provider communication. Hospitalists carry the lift of being leaders in patient care, ensuring that communication is efficient between all teams, especially with consulting clinical specialists who are providing services to the patient. Strong communication between the hospitalist and consulting clinical specialist(s) ensures optimal patient outcomes and satisfaction. Timely communication, along with increased frequency and standardization of information, supports successful transitions of care and care coordination during admission and prior to patient discharge.
On the other hand, poor communication between physicians can significantly hamper medical progress and delay advancements in collaborative efforts. One important study regarding physician-to-physician communication indicates that only a very small percentage of physicians providing primary care engage in direct contact with subspecialty clinical consultants. Even more surprisingly, an overwhelming percentage of consultants completely neglected to notify the referring physicians of the results of their findings. Such challenges directly affect patient care and pose the risk of further complicating the patient's condition (McPhee, 1984). Another study shows the potential for lack of or delayed communication to possibly result in detrimental consequences. The study found that patients were sometimes released from hospitals before all of their medical tests had even been completed (Roy, 2005). Other consequences of gaps in communication may lead to patient harm, continuation of incorrect treatment, increased length of stay, and increased costs.
As stated by Taran (2011), a breakdown or delay in communication has the potential to result in further complications in the health of the patient with consequential outcomes. Without effective and timely communication between physicians, both the quality of care and the patient experience can suffer.
Engage in direct, verbal communication whenever possible
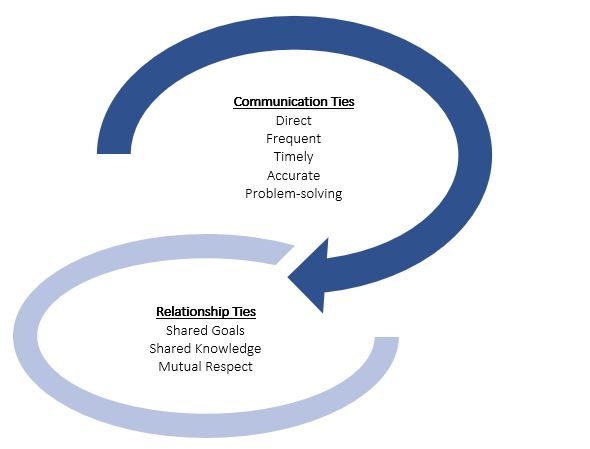
The American Academy of Family Physicians has developed a few guidelines that can assist in improving the communication between physician-to-physician contact. It is important to highlight that recommendations suggest that as the lead provider in the patient care, the hospitalist should be accessible to discuss the patient's medical problems and changes as they present in a timely manner. Timely and direct communication between the hospitalist and subspecialty clinical consultants concerning change in status, test results or new diagnosis, and any complications is extremely important.
One of the ways that Anasuya Brahmamdam, M.D., manages communication with clinicians outside of the hospitalist team is by consistently striving to develop a relationship with the care partner(s). Upon entering a consult order, she documents it in the patient electronic medical record and follows up with a personal call to the provider for hand-off. Communication back to the patient includes the specifics of her encounter and includes language such as, “I have consulted with Dr. X from Neurology. Their findings include ABC and recommendations are 123. Does this sound correct to you?”. Using this language ensures that the patient hears that we are working together collaboratively to ensure that their presenting issues are carefully being reviewed and addressed.
Mohamed M. Bakr, M.D., offers another example when he works with oncology subspecialty clinical consultants. When following up with patients, he uses language such as, “I realize your conversation with your oncologist was hard on you and you have a lot of questions and concerns. Tell me what you are worried about and how can I help you feel better?” Asking open-ended questions allows patients to feel heard and their concerns to be better addressed on their terms.
Call-to-Action: Timely, direct and effective communication between physicians is especially vital to patient care and patient satisfaction. The HCAPHS physician communication category decreased by 20 percent from 2019 to 2020, with JSUMC ranking at the bottom 12th percentile nationally. This data highlights the need for us to strengthen our physician-to-physician practices. Moving forward, we ask that you commit to openly communicating with all of our subspecialty clinical consultants to obtain the best and safest possible outcome for the patient. We ask that you:
1 – Let your patient know that you will be connecting to their specialists;
2 – Communicate directly with the consulting specialist; and,
3 – Provide follow-up and direction in the plan of care after consulting with the assigned specialist.
Together, we will improve and offer the best possible care to our patients.
References
- McPhee SJ, Lo B, Saika GY, Meltzer R. How good is communication between primary care physicians and subspecialty consultants? Arch Intern Med. 1984 Jun; 144(6):1265-8.
- Roy CL, Poon EG, Karson AS, Ladak-Merchant Z, Johnson RE, Maviglia SM, Gandhi TK. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005 Jul 19; 143(2):121-8.
- Taran, S. An Examination of the Factors Contributing to Poor Communication Outside the Physician-Patient Sphere. Mcgill Journal of Medicine. 2011 Jun; 13(1): 86. Retreived from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3277343/
